Detached Retina
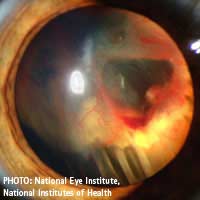
Detached retina is a serious condition that can lead to blindness if it is not diagnosed and treated very quickly. It affects about one in 10,000 people.
The retina is the innermost layer at the back of the eye that performs much the same function as the film in a camera. It contains millions of tiny light receptors that convert the visual image formed by the eye’s optical system into electrical impulses. These are then relayed along the optic nerve to the brain to complete the seeing process.
In certain circumstances it’s possible that the retina can become detached from its underlying layer the choroid, which contains the many blood vessels that provide the retina with its nourishment. When this happens, vision in the affected region is lost. The retina may also become torn at the point of detachment. The situation can be exacerbated if fluids such as blood or vitreous fluid from the space in front of the retina penetrate beneath it.
The Causes of Detached Retina
Some people are more susceptible to detached retina than others. The groups most at risk are:- Middle-aged or older people
- Those with a family history of retinal detachment
- Severely short-sighted (near-sighted) people, where the eyeball is elongated and the retina is ‘stretched’ and is thinner than normal
- Cataract patients. The presence of scar tissue following a cataract operation leaves the retina or its bond with the underlying choroid weakened. This can also happen as a result of other types of eye surgery
- Diabetes sufferers. This group may develop a condition called diabetic retinopathy, where blood vessels underneath the retina weaken and rupture. The resulting leakage of blood can cause the retina to lift from the choroid
- Victims of ‘blunt trauma’ in the region of the eye, usually as the result of an accident
Symptoms of Detached Retina
Since a detached retina is painless, the first symptoms are likely to be visual abnormalities, most commonly:- Full or partial loss of the field of vision. This is rather like a curtain or veil falling over part of the eye
- “Floaters”. Most people experience dark, tadpole-like “floaters” from time to time, but the sudden and sustained appearance of floaters is cause for concern
- Brief flashes of light in the eye
- A sudden change or blurring of vision. The cornea and the lens in the eye focus the image on the retina. If part of the retina has moved, the image at that point will be blurred
Treatment of Detached Retina
Once the retina has become detached, it needs to be surgically repaired to restore or arrest loss of vision. If the detachment is partial a special type of laser treatment called photocoagulation can be used. This treatment creates a scar around the edge of the retinal hole, fusing the retina to its underlying layer and preventing the entry of damaging fluids.An ophthalmologist (eye surgeon) may use another technique known as scleral buckling. This involves sewing one or more silicone bands to the outside of the eyeball, causing the wall of the eye to ‘buckle’ inwards and to bridge the retinal hole. In most cases the retina will then reattach, although there is usually an increased degree of short sightedness because the eyeball is lengthened by the procedure.
Another method of repairing a retinal detachment is called pneumatic retinopexy. The perimeter of the retinal hole is fixed by freezing or by laser treatment. A bubble of gas is then injected into the eye and the position of the patient’s head is adjusted so that the bubble is resting against the hole. This is not the most practical of treatments because the patient has to keep the head in the same position for perhaps several days until the retina reattaches through natural processes!
There’s really no way to prevent a retinal detachment, but regular visits to the optometrist will ensure that this and other eye problems are detected in the early stages, and have the best possible chance of successful treatment. People with diabetes, however, can minimise the possibility of detached retina caused by diabetic retinopathy through careful control of their blood sugar levels and by having eye checks through dilated pupils at least once a year.
Finally, the correct eye protection should always be worn in hazardous environments!
- What is Allergic Conjunctivitis
- What Does Uveitis Mean?
- What is Retinal Vein Occlusion, RVO
- My Lazy Eye Got Me Bulllied at School
- Iritis Explained
- Squint Repair
- Amblyopia or Lazy Eye
- Blepharitis
- Chalazion or Lump on Eyelid
- Styes
- What is Age Related Macular Degeneration?
- Treating Cataracts
- Short Sightedness
- Treating Age Related Macular Degeneration
- Diabetic Retinopathy
- Long Sightedness
- Astigmatism
- What are Cataracts?
- Treating Glaucoma
- What is Glaucoma?

Re: Contact Lens Trials Explained
Hi, I just visited eyehelp.co.uk and wondered if you'd ever thought about having an engaging video to explain what you…
Re: Is There an Operation for 'Lazy Eye'?
written on the parchment was scratched out
Re: What is Vitrectomy Surgery?
I had vitrectomy 4 weeks ago. The surgery was not well done as apparently bleeding occurred. The hole did not close despite having…
Re: Glasses or Contacts?
I need a eye exam and new glasses it's been since 2013/ I have no income I lost my boyfriend last September and I've been homeless ever…
Re: Eyewear for the Partially Sighted
This extract from your text is not clear and the grammar is poor- and the letters in the validation box are mixed…
Re: Eye Cancer Symptoms
I have yellow in both eyes lools like 2 dots. But looks like its makin the white part of my eye yellow whats wrong with me
Re: Are my Glasses Affecting my Eyes?
Hi, Please can anyone give advice on wearing varifocals. After a short while I develop a severe ache in my left eye and…
Re: Are my Glasses Affecting my Eyes?
On wearing my new varifocals, I am finding that my left eyeball hurts so much it feels like it will explode after 15…
Re: What is the Cause of my Itchy Eye?
I have One and only One itchy eye that has been going on 24/7 for 5 weeks.Eye is not swollen vision not affected. Eye doc…
Re: Contact Lens Trials Explained
Hi, We wanted to get in touch with you to increase traffic on your website. Please reply to this email so we can send you free…